Why VBC Makes Healthcare More Expensive
TLDR: Value Based Care is a Risk Based Contract With Unintended Consequences
Let’s start with an uncomfortable fact.
After fifteen years of Value-Based Care as national policy — ACOs, MSSP, bundled payments, CMMI models, and everything downstream of the Affordable Care Act — national health expenditures as a percentage of GDP have not decreased. In fact, they have continued to climb.1
Meanwhile, CMS, Aledade, and other organizations consistently point out that ACOs are a success and generate “shared savings.” In fact, the ACO my practice is part of has also consistently generated “shared savings,” and I have personally received these bonus payments.
The paradox is that both statements are true:
ACOs are achieving “shared savings.”
VBC is raising the total cost of care (TCOC).
The central question most people struggle with is “how?”
How is it possible that Value-Based Care, which is supposed to reward physicians for not performing unnecessary tests and procedures, is actually increasing TCOC?
The short answer:
In its dominant form, VBC shifts financial risk and administrative burden onto practices, which favors consolidation.
Once consolidation occurs, the consolidated health organizations raise prices and extract revenue from every payer stream it touches.
Furthermore, the “savings” in Medicare ACO contracts are compared to a “fictional” benchmark, which can be gamed using risk coding and other mechanisms.
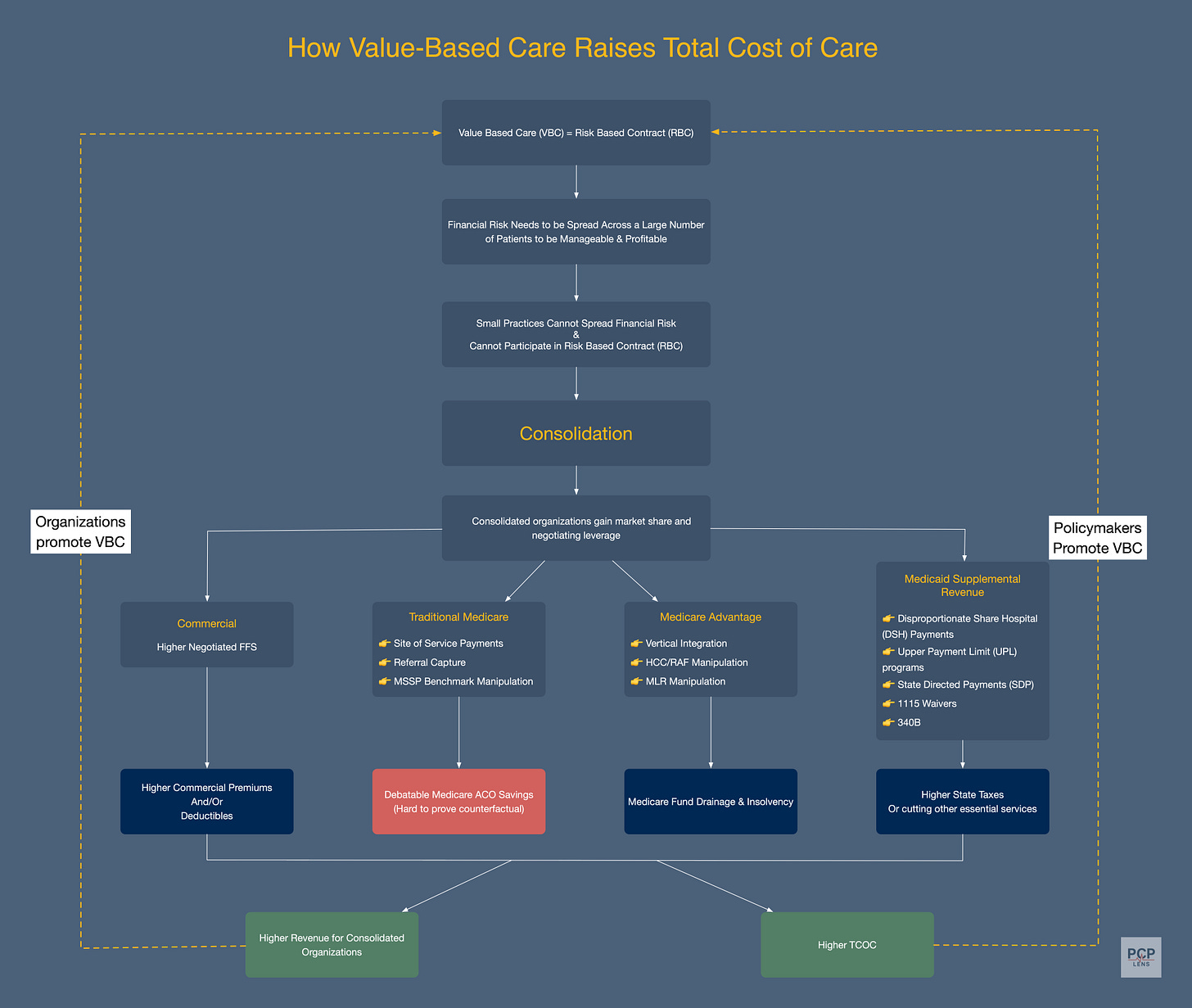
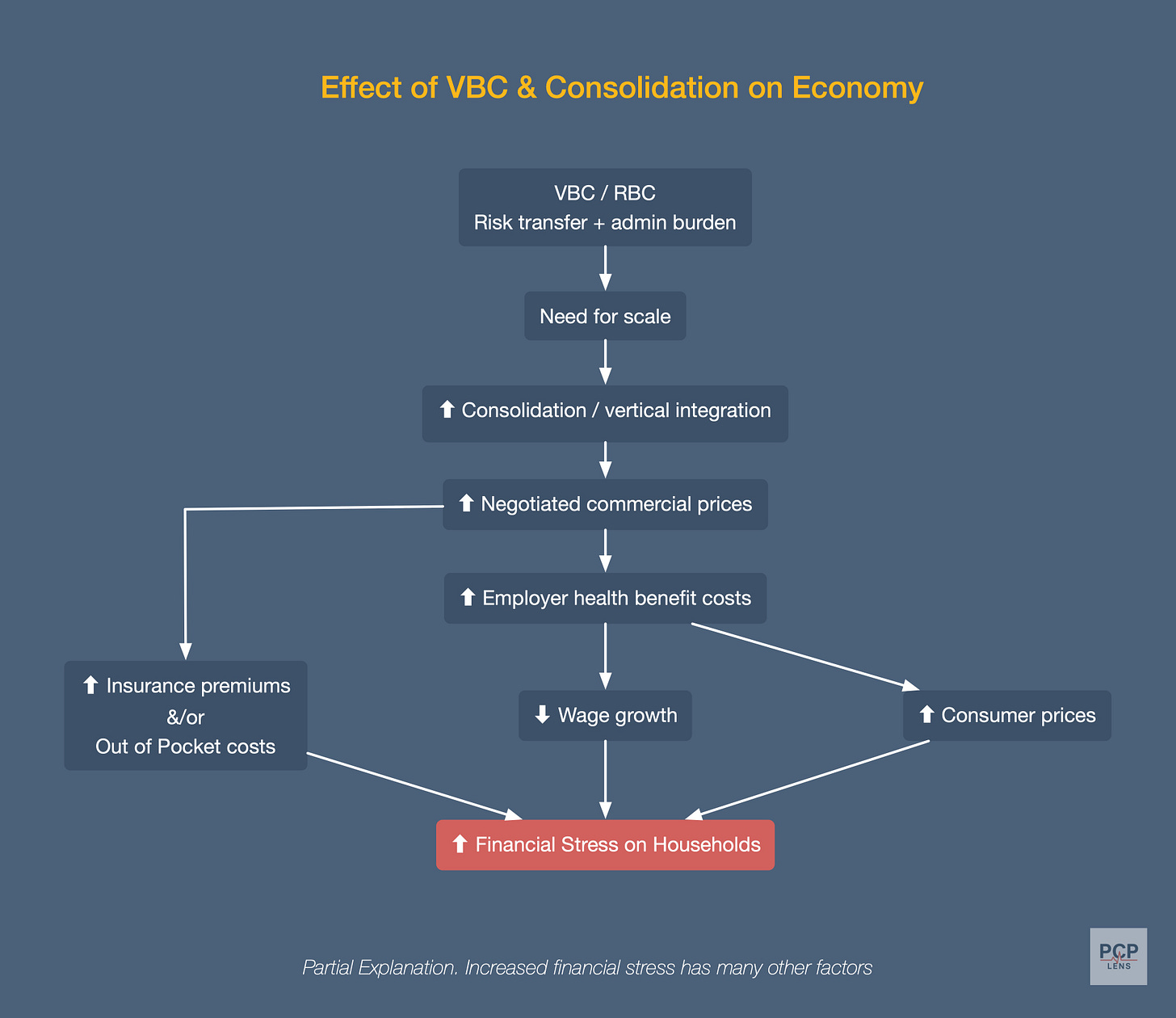
The flowchart above summarizes the mechanisms by which VBC/RBC increases the total cost of care for the entire system. This is the entire gist of the article. If you understand this flowchart, please share it with your colleagues.
For more details, let’s dive in.
The Pre-VBC Pressure Stack
Before VBC existed, independent primary care was already being squeezed, and consolidation had already started. This consolidation pressure came from a stack of policies that accumulated over three decades:
RBRVS budget neutrality (1992–present): When CMS updates the physician fee schedule, any increase is offset, generally by reducing the conversion factor2. This budget-neutrality mechanism has compressed the physician fee schedule for decades. The AMA estimates that, on average, physician fees have declined by 33% (adjusted for Medical Economic Index Inflation) since 2001.
HITECH / Meaningful Use (2009): Required EHR adoption, which created huge IT infrastructure costs for practices.
PQRI → PQRS → MIPS (2007–present): A growing list of quality reporting requirements since the early 2000s, which not only added to the administrative burden but also financially penalized small practices that were unable to submit data.
General compliance overhead: HIPAA, OIG, payer credentialing, prior authorization processes, and a slowly expanding regulatory surface area.
All these costs and administrative pressures were already squeezing independent practices, and then came VBC.
The Step Change: Value = Risk
The key reason why VBC was a step change in consolidation pressure is that the name “Value-Based Care” is a misnomer. In my VBC simulation model, I showed how contracts matter more than care.
Most of VBC is implemented as “Risk-Based Contracts” (RBC).
When a small practice signs an RBC, it is taking on a financial risk for the patient population the physician serves. This is not a function of the physician’s care, but a function of insurance. This means that your physician's office is now acting as an insurance company.
And for an insurance company to be profitable, it needs a large pool of patients to spread the risk, so that a few high-cost patients don’t wipe out the entire financial pool.
In real life, if I have a few cancer patients in my practice who need expensive treatments, there is no way I can spread that risk across my entire patient population.
This is not a problem that can be solved by working harder, practicing better medicine, or lowering overhead. Insurance is a mathematical model - given the “benchmark,” either you have the scale, or you don’t. There is no workaround.
In a nutshell, risk requires scale. The larger the pool of patients, the higher the probability of succeeding in RBCs
Aside: Benchmarks Are Relative, Not Absolute.
An ACO “saves” money if its actual spending is below its benchmark. The benchmark is constructed from historical regional spending, often adjusted upward for national trend factors. These benchmarks can be manipulated using several mechanisms, including HCC manipulation, cherry picking both doctors and patients, cost shifting to non-contracted providers, changing Tax IDs etc.
Since it is very hard to prove the benchmark counterfactual (i.e., what costs would be without ACO), beating the benchmark is not the same as reducing the cost of care.
The correct answer, we don’t know if VBC/RBC saved any money.
The Consolidation Response
Given the fact that RBC requires scale, the only option left is to consolidate. I subdivide consolidation into two categories:
Hard Consolidation:
Physician employment: Hospitals and health systems employing primary care and specialty physicians directly.
Hospital M&A: Health systems acquiring each other, producing regional giants with dominant market share and scale to take on RBC.
Vertical integration: Payers acquiring provider groups (e.g., UnitedHealth/Optum), or provider systems launching health plans.
Private equity roll-ups: PE-backed platforms acquiring independent practices to aggregate scale for VBC contracting, specialty leverage, or both.
Soft consolidation:
ACO networks, such as Aledade, aggregate thousands of otherwise-independent primary care practices into shared MSSP contracts.
Soft consolidation is interesting because it's often framed as the alternative to hard consolidation. “You don't have to sell to the hospital — you can join an independent ACO such as Aledade and stay independent.”
And independent ACOs are a great way to stay independent. I know that, because I am a member of one. But independent ACOs require dollars to manage risk.3 Since ACOs don’t have as diversified revenue streams (compared to large health systems), the money has to come from somewhere. Physician practices that have been squeezed for decades don’t have those dollars. So eventually, these independent ACOs will need to partner with someone:
VC or traditional investors: e.g., Aledade, ChenMed,
Hospital system. e.g., via a physician hospital organization (PHO),
Payors: e.g., Oak Street is a wholly subsidiary of CVS/Aetna
Private equity
The question for all these soft consolidation models is whether they will eventually be acquired by their funders.
VBC does not primarily solve the cost problem. It reorganizes who bears accountability and who captures revenue, i.e., it moves dollars away from practicing front-line physicians to large systems, while blaming them for rising healthcare costs.
The Financial Fruits of Consolidation
Consolidation does not just make your favorite indie doctor disappear. It unlocks a specific set of revenue-capture mechanisms that either require scale or exploit loopholes in government programs. Let’s look at a few of them across different payor types.
Commercial
Consolidation and scale translate into higher negotiated leverage with commercial health plans. There is plenty of evidence to support that when health systems consolidate, prices go up, while quality and access either stay the same or get worse.
These higher healthcare costs in the commercial market manifest in various ways:4
Higher healthcare premiums and/or higher out-of-pocket costs, such as copays and deductibles
Higher employer costs (as they pay part of the healthcare premium)5
Lower salaries (or not getting a raise)
Higher prices, such as groceries or Starbucks coffee
So the unintended consequence of VBC and consolidation is that it may contribute to higher prices and limited purchasing power, pushing people into poverty!6
Traditional Medicare
Site-of-service payment differentials. When a physician practice is acquired by a hospital and redesignated as a hospital outpatient department (HOPD), the same service billed by the same physician for the same patient gets a facility fee added on top, which can be anywhere from 20%-25% for office visits to 200-400% for procedures.7
Referral capture. Consolidated systems route referrals internally to their employed specialists, imaging centers, and labs. Acquiring independent PCPs means locking in downstream revenue that an independent PCP would have distributed across multiple specialists (both independent and hospital-employed).8
MSSP benchmark manipulation. This is a whole topic on its own (although CMS has been cracking down on benchmark manipulation).
Medicare Advantage
Plan-provider vertical integration. When a provider system owns the MA plan9 (or vice versa), it can move money internally between its various subsidiaries to bypass Medical Loss Ratio (MLR) requirements and hide profits.10
Coding intensity. MA plans are paid based on the HCC (Hierarchical Condition Category) risk scores of their enrollees. They can manipulate these risk scores to artificially inflate the benchmark, which I discussed in a previous article, “How Much is Your Diagnosis Worth?”11
Medicaid
Medicaid is often ignored in VBC/RBC discussions because it has historically had the lowest reimbursement rates. What most people don’t realize is that State Medicaid programs have a lucrative supplemental payment architecture,12 including:
Disproportionate Share Hospital (DSH) payments
Upper Payment Limit (UPL) programs
State-directed payments under managed care
1115 waiver pools
340B drug pricing program
These are pools of state and federal dollars that flow preferentially to safety-net and other qualifying systems, that reimburses health systems indirectly for taking care of Medicaid and non-insured patients. Independent practices do not qualify for these programs. So when VBC/RBC pressures force independent practices to sell to large health systems, those systems now capture the supplemental payments listed above, raising the total cost of care for Medicaid.
The Paradox of Savings
A consolidated system might report MSSP ACO savings against its Medicare benchmark while simultaneously raising commercial prices, extracting federal and state dollars through site-of-service differentials, and collecting supplemental Medicaid payments. They just measure different things.
Savings Are Contract-Specific; Costs Are System-Wide
The Medicare ACO savings may be real, or they may be illusory. However, the dollars from other sources are real.
Conclusion
Given that there has been some success (and I would argue that that success is debatable) with VBC, there is a strong incentive to “improve” it. This improvement ends up taking a few forms:
Bring more doctors into risk contracts
Increase administrative oversight to ensure only “good” care is being delivered
Make ACOs (aka PCPs) take on more financial risk
And, all these factors increase consolidation.
The only way to manage this risk is for providers to become payors, and for payors to become providers, aka, vertical integration, where everyone is a “payvidor.”
We are already entering an era where, in many regions, there are only 1-2 regional healthcare systems and/or health plans. Soon, there will be only a handful of national payvidors who define, decide, and deliver healthcare at ever-higher prices.
Is this what we want for the future of healthcare?
Centers for Medicare & Medicaid Services. (2025). National Health Expenditure Accounts: Historical. https://www.cms.gov/data-research/statistics-trends-and-reports/national-health-expenditure-data/historical
Keehan, S. P., Fiore, J. A., Poisal, J. A., Cuckler, G. A., Sisko, A. M., Smith, S. D., Madison, A. J., & Rennie, K. E. (2025). National health expenditure projections, 2024–33: Despite insurance coverage declines, health to grow as share of GDP. Health Affairs, 44(7). https://doi.org/10.1377/hlthaff.2025.00545
The second article was
The Conversion Factor (CF) set by CMS for Medicare converts RVUs into dollars.
I have a simulation model that shows the infrastructure costs required to build and run an ACO, as well as how contracts are reconciled. You can find it here:
Baicker, K., & Chandra, A. (2006). The labor market effects of rising health insurance premiums. Journal of Labor Economics, 24(3), 609–634 (https://doi.org/10.1086/505049)
Brot-Goldberg, Z., Cooper, Z., Craig, S. V., Klarnet, L. R., Lurie, I. Z., & Miller, C. (2024). Who pays for rising health care prices? Evidence from hospital mergers (NBER Working Paper No. 32613). National Bureau of Economic Research (PDF Link)
Kanimian, S., & Ho, V. (2025). U.S. medical prices and health insurance premiums, 1999–2024. JAMA Network Open, 8(12), e2547462
Hager, K., Emanuel, E. J., & Mozaffarian, D. (2024). Employer-sponsored health insurance premium cost growth and its association with earnings inequality among U.S. families. JAMA Network Open, 7(1), e2351644 (https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2813927)
Capps, C., Dranove, D., & Ody, C. (2018). The effect of hospital acquisitions of physician practices on prices and spending. Journal of Health Economics, 59, 139–152. https://doi.org/10.1016/j.jhealeco.2018.04.001
Bipartisan Policy Center. (2025). Site neutrality in Medicare payment. https://bipartisanpolicy.org/issue-brief/site-neutrality-in-medicare-payment/
Lin, H., McCarthy, I. M., & Richards, M. (2024). The effects of physician vertical integration on referral patterns, patient welfare, and market dynamics. Journal of Public Economics, 238, 105183. https://doi.org/10.1016/j.jpubeco.2024.105183
Although uncommon, there are several large systems that have their own MA plans e.g, UPMC
Geruso, M., & Layton, T. (2020). Upcoding: Evidence from Medicare on squishy risk adjustment. Journal of Political Economy, 128(3), 984–1026. https://doi.org/10.1086/704756
Medicare Payment Advisory Commission. (2024). Report to the Congress: Medicare payment policy (Chapter 13: The Medicare Advantage program). https://www.medpac.gov/wp-content/uploads/2024/03/Mar24_Ch13_MedPAC_Report_To_Congress_SEC.pdf
The transition from V24 to V28 is designed to curb some of the HCC manipulation.
Medicaid and CHIP Payment and Access Commission. (2024). Medicaid base and supplemental payments to hospitals. https://www.macpac.gov/wp-content/uploads/2024/05/Medicaid-Base-and-Supplemental-Payments-to-Hospitals.pdf