The Math Behind Hospital-Based ACOs
Exposing the structural trap with the VBC Simulation Model
In my last newsletter (and video), I shared the VBC Financial Simulation Model and explained how Value-Based Care contracts work in real life.
If you have not “played” with the simulation model, I highly recommend that you do so using the link below.
In this article, I use the simulation model to show why hospital-based ACOs are structurally stacked against independent PCPs.
Let’s dive in.
The video version of this article is embedded below and available on my YouTube Channel.
The audio podcast and video versions are also available on the Podcasts Page.
The Simulation Model
There are 7 steps in the model. Each step has several variables that the user can adjust. I have made baseline assumptions for each variable, including worst-case, realistic, and best-case scenarios. In addition, many variables include tooltips that explain their meaning.
For this article/demonstration, I will follow the realistic scenario in the VBC Simulation Model.
Steps 1-3
The steps are the same as in my last article. They include:
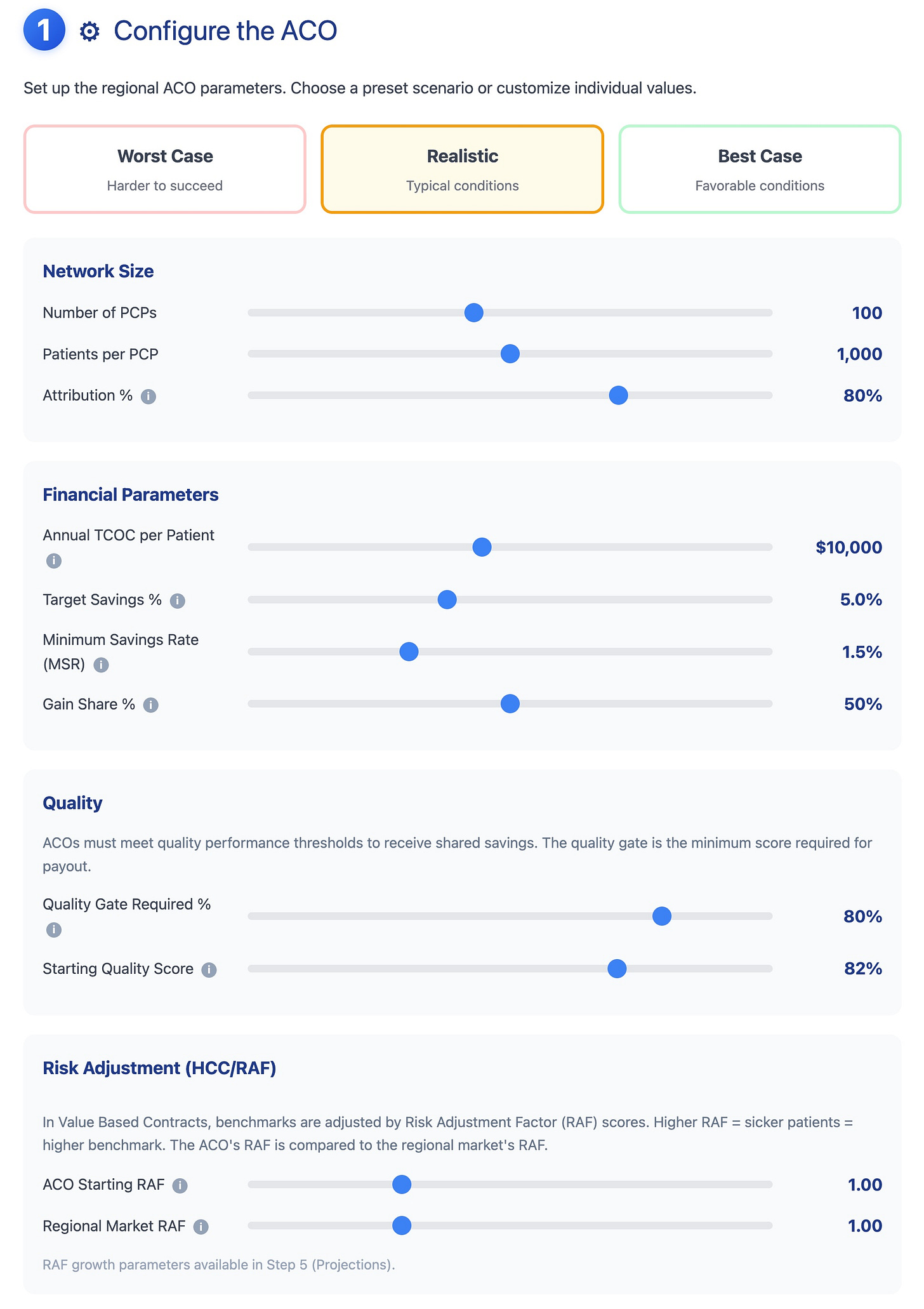
Setup: Allows the user to choose the ACO size and baseline contract terms.
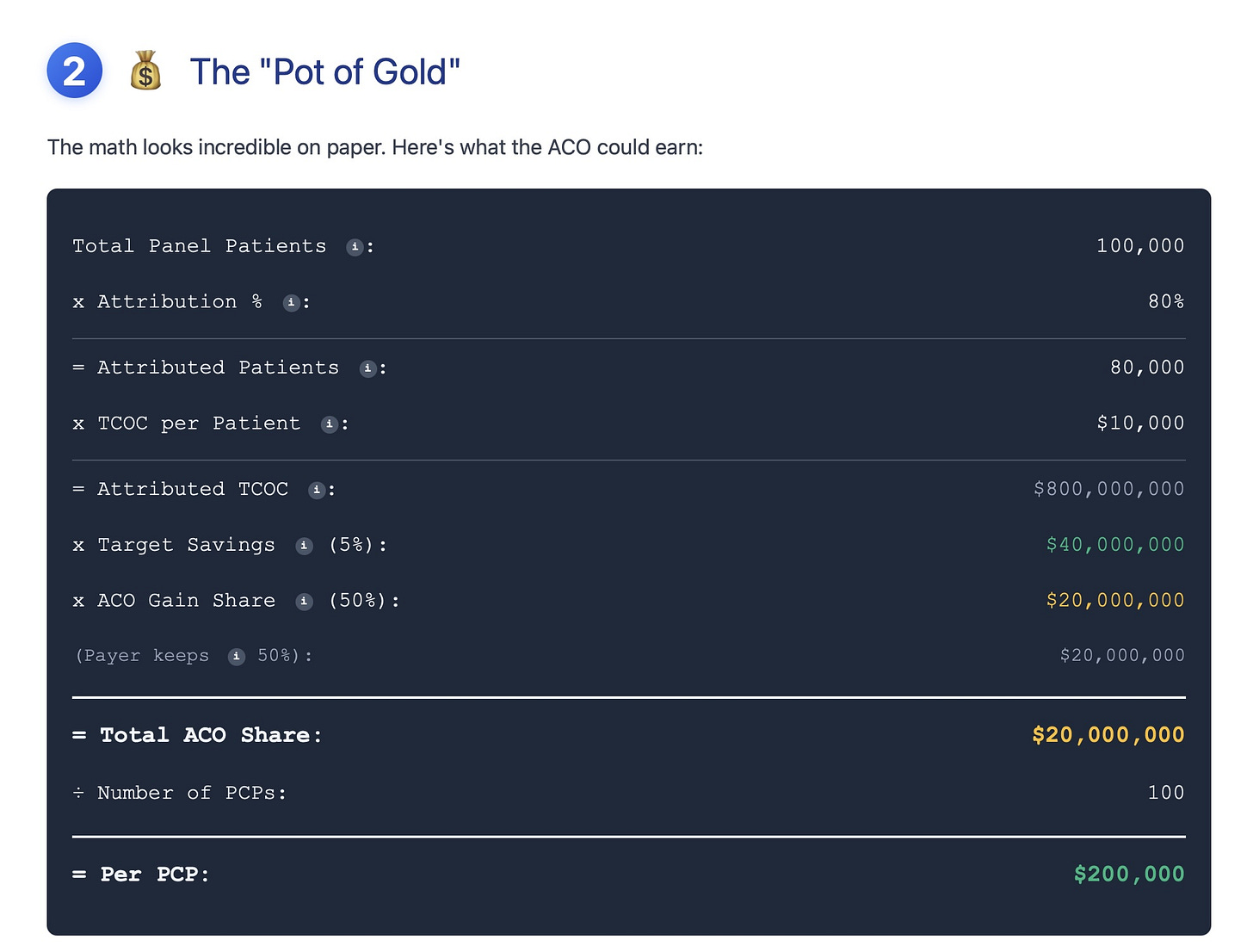
Opportunity (Pot of Gold): Shows the back of the envelope ACO savings opportunities based on the assumptions in Step 1.
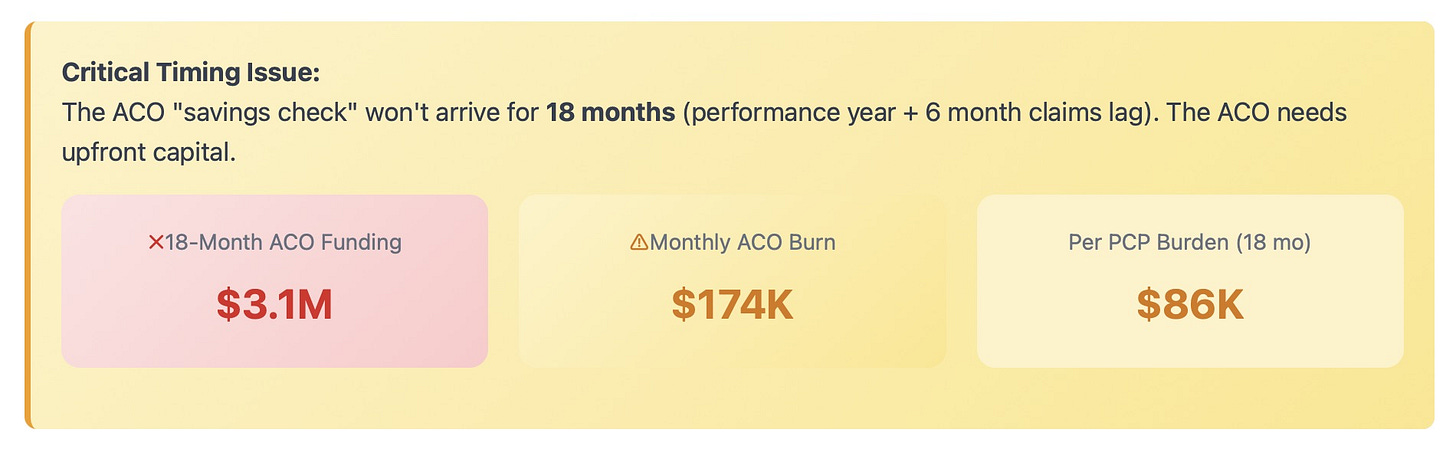
Reality Sets In: Simulates the costs of setting up the ACO. This step also includes the PCP's financial burden from the added administrative tasks.
By the end of Step 3, our newly formed ACO needs approximately $3.1 million for the first 18 months to function. In addition, individual PCPs have lost the opportunity to earn approx $86K in these 18 months.
Step 4: The Funding Decision
With $3.1M needed to operate the ACO, the next question is: who provides the capital? In this step, we decide which funder to choose from:
Bank Loan
Hospital partner
Payer Advance (as pmpm)
Private Equity
As we will focus on hospital-based ACOs in this article, we will choose Option B: Hospital Partner.
Hospitals (more precisely, large health systems) can form ACOs in two broad ways:
Fully owned ACO with employed clinicians and facilities.
Partnership model, which is often structured as a joint venture (JV) between the hospital and the ACO. This JV is often called a “Physician Hospital Organization” or PHO. The hospital provides funding to run the PHO, which then contracts with payors.
This simulation focuses on the second model, i.e., PHOs. This structure allows an independent ACO to sign risk-based contracts while the hospital supplies the capital the ACO needs to operate.
In practice, hospital funding usually comes with two negotiated terms:
A share of ACO gains, aka gainshare: the model’s realistic scenario uses a 50/50 split between the hospital partner and the ACO.
Redirecting referrals (volume capture): The hospital partner, as a condition of funding, will require independent PCPs to redirect a portion of their referrals to hospital-employed physicians and hospital facilities.
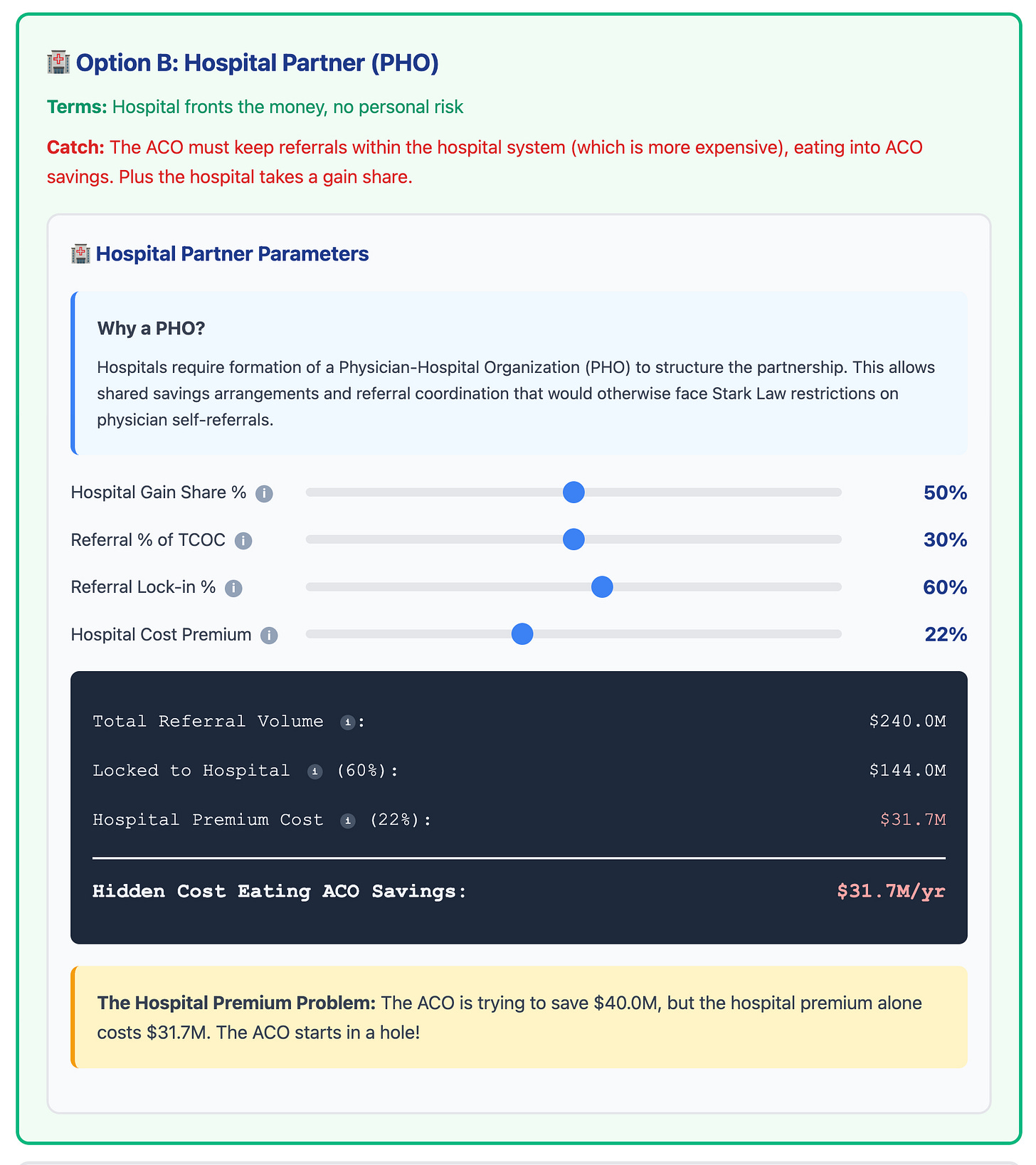
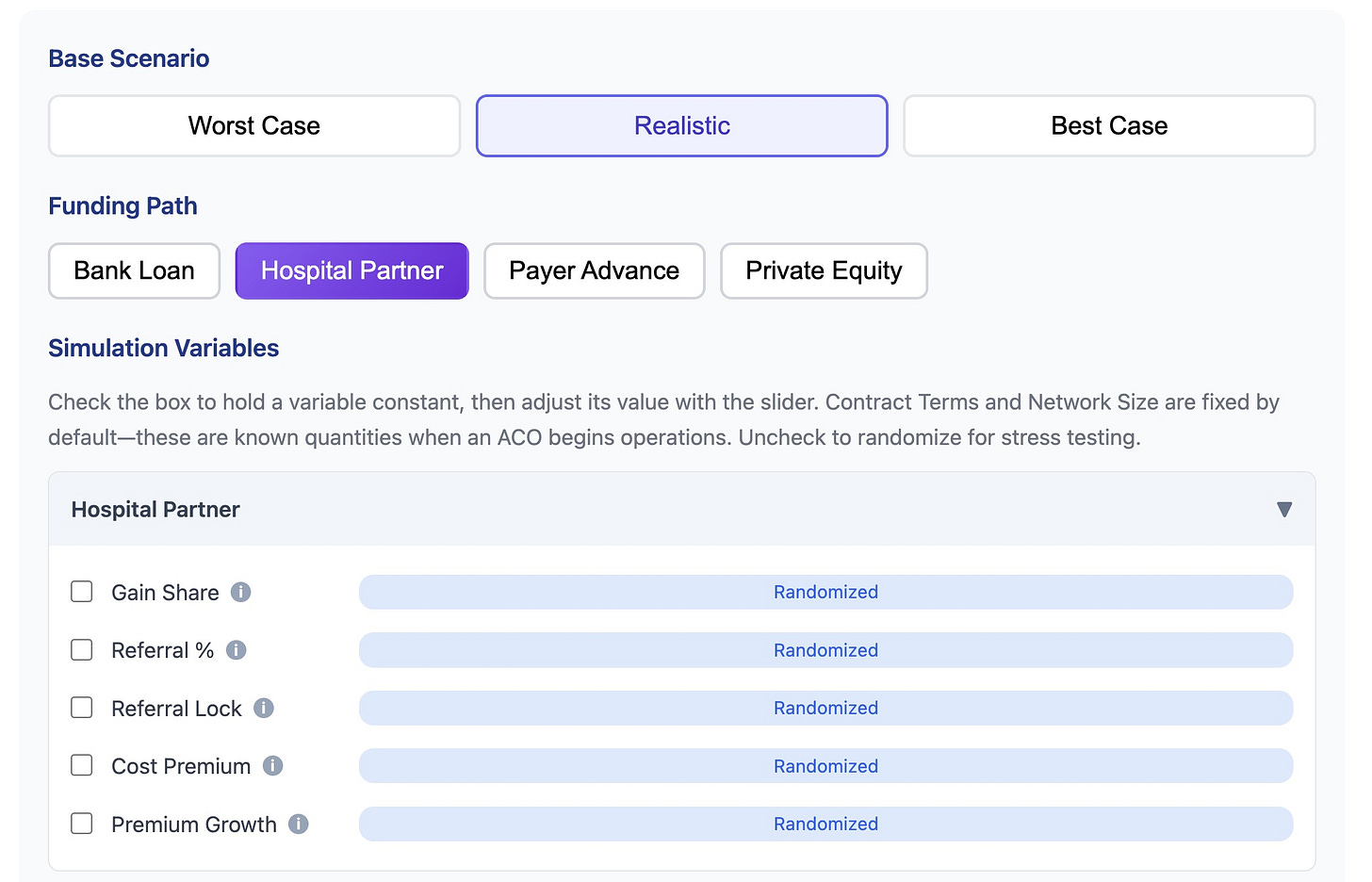
Let’s look at the variables and math from the screenshot above.
Hospital Gainshare: This is pretty straightforward. The hospital negotiates a share of any ACO savings.
Referral % of TCOC: This is an approximation of the percentage of TCOC that can be attributed to downstream referral costs.
Referral Lock-in %: This is what the hospital partner wants independent PCPs to redirect to hospital-employed physicians and facilities.
Hospital Cost Premium: This approximates how much more expensive it is for patients to receive care at hospital facilities vs independent specialists. For Medicare Advantage, this is driven predominantly by facility fees, while for commercial plans, it is driven by higher negotiated fee-for-service rates.
Based on the realistic scenario in the model, let’s do the math:
Based on the math, you can clearly see that the ACO's success requires lowering the TCOC by $40M in the realistic scenario (see Step 2 image above), but redirecting referrals raises the TCOC to the point of erasing any shared savings.
Hospital ACO tradeoff: the same terms that “fund” the ACO can destroy shared savings.
Furthermore, the PHO JV provides a safe harbor from Stark and anti-kickback laws by creating an exempt entity called a “Clinically Integrated Network” or CIN.
Now that we have chosen a funder and understand the tradeoffs, let’s look at 1st year outcomes.
Step 5: 1st Year Outcomes
Given that hospital referrals cost the ACO approx $31M, the ACO will not meet their 1.5% MSR target in the realistic scenario to receive any shared savings.
Since the ACO will not receive any shared savings, the PCPs lost approx $86K in the last 18 months. This may have a devastating impact on some small PCP practices and nudge them to sell/join the hospital.
But, you may ask, what about the hospital? The hospital also lost its $3.1M investment in the ACO. That is not the case, for three reasons:
For $3.1M investment, the hospital received approx $31.7M in referral revenue.
Furthermore, for PCPs who decided they lost enough money and joined the hospital will bring in approx $1-2M/year
The following year, the hospital will go to commercial payors and negotiate higher fee-for-service rates.
All three factors increase TCOC.
Furthermore, if the ACO succeeds in reducing TCOC, the hospital takes a portion of shared savings, along with all the referral volume!
Step 6: Project Outcomes
In the realistic scenario, the ACO is bound to fail in the 1st year. Therefore, there is no outcome to project out. You can modify the simulation parameters (e.g., use the best case scenario) to see the projections.
Step 7: Monte Carlo Simulation
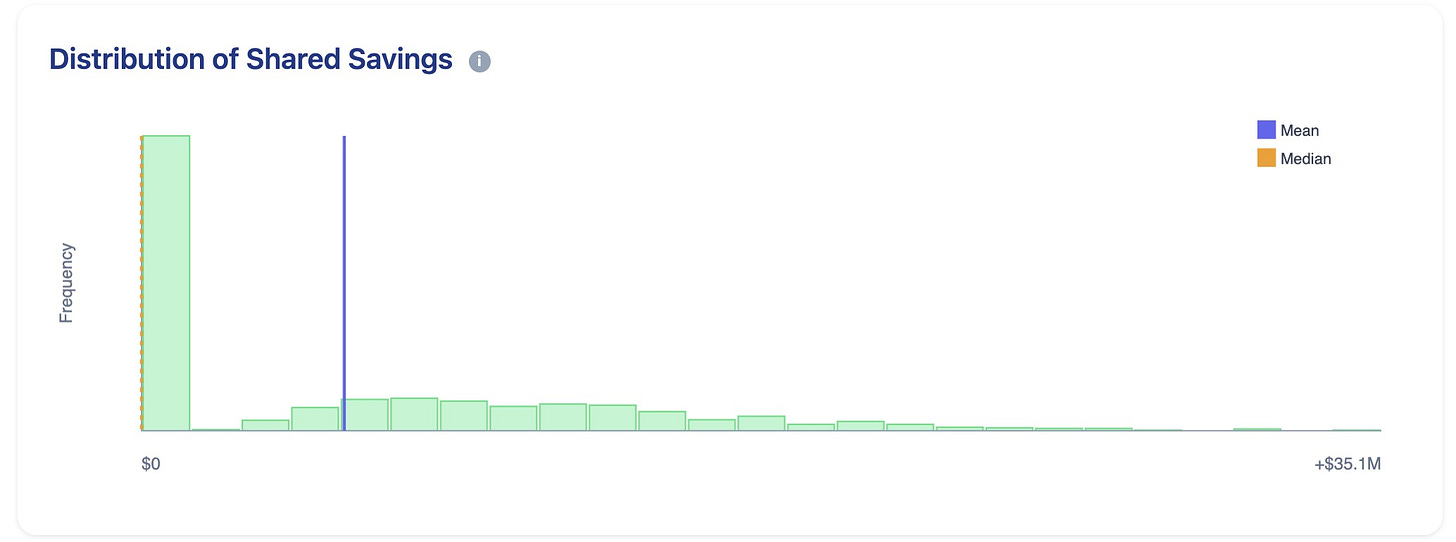
The defaults for the realistic-scenario Monte Carlo simulation are to randomize all hospital variables.
When you run the simulation, it shows that the ACO fails almost half the time. The screenshot shows that, in the vast majority of cases, the ACO will receive a $0 payout!
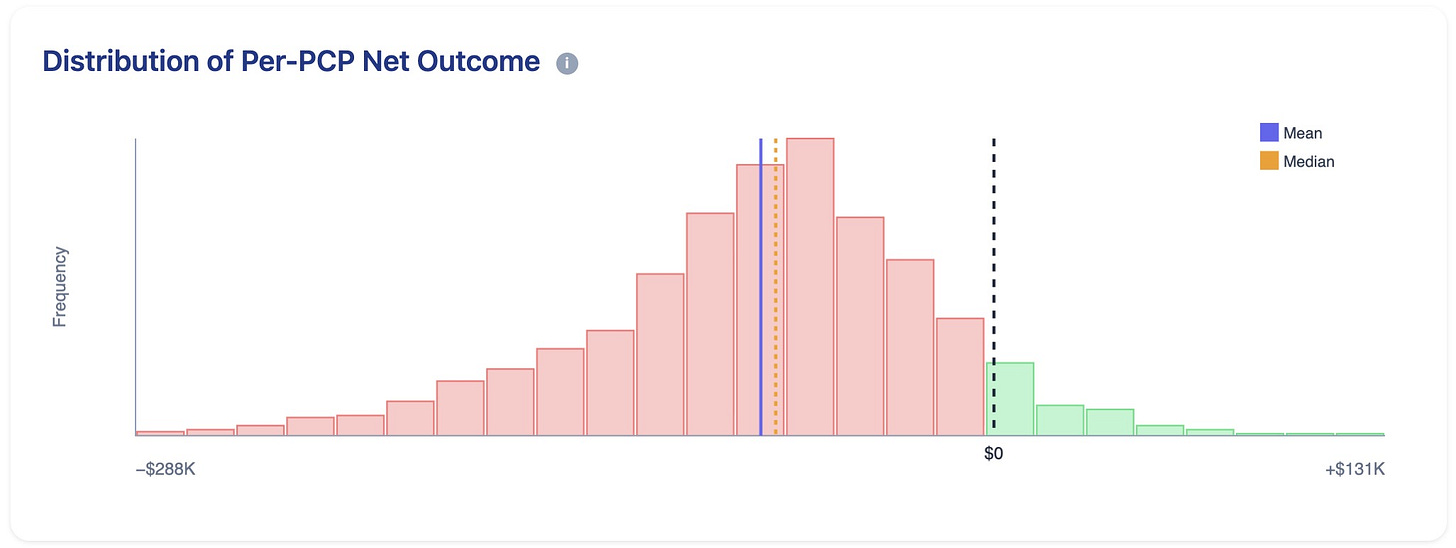
The picture is even worse for PCPs. Their probability of losing money is approx 94%.
Final Thoughts
As you can see from the simulation, the probability of PCPs losing money and doing administrative work under VBC is pretty high.
Hospitals form ACOs for 2 reasons:
To show that they are participating in value-based care
They’re a legal, structured mechanism for them to expand market share, capture referral revenue, and consolidate the physician workforce.
The VBC model is structurally designed to benefit hospitals and large systems at the expense of small PCP practices. And we continue to wonder why small independent practices are disappearing.
The link to the model is below. Please leave a comment with your thoughts and suggestions.